By Astrid Graterol on Nov 14, 2019 @ 02:43 PM
According to the American Diabetes Association (ADA), people with type 1 diabetes are at higher risk for eye complications. When most people think of diabetes, they think of sugar levels and are not aware of the effects it has on different organs of the body, including the eyes. In order to understand the connection between diabetes and vision, it helps to understand how the eye works.
The cornea is a transparent structure found in the front of the eye that helps to focus on incoming light, that light passes through a protective layer called aqueous humor and then through the crystalline lens that allows for more focusing, then finally it hits the retina. The retina is specialized for seeing the fine details and it is supported by blood vessels. A visualization is shown below.
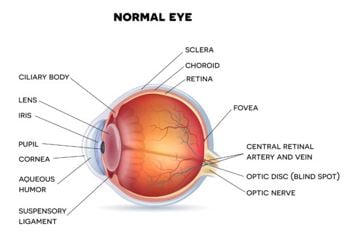
Now, where is the connection? Diabetes creates high blood sugar (glucose) levels, which causes glucose to collect in the bloodstream. The glucose then narrows the blood vessels, reducing the flow of blood and oxygen, which increases the risk of damaged vessels. This can lead to short-term and long-term vision complications.
Short-term
Damage to small blood vessels can lead to the most common short-term vision problem, blurry vision. Blurry vision can occur because of:
- Swelling- High blood sugar can cause irritation to the eye lens, causing it to swell. The swelling changes the shape of the eye, which leads to blurry vision.
- Hypoglycemia- A crash in low blood sugar can lead to negative impacts on brain function, which can cause blurry vision.
Eye and vision complications from diabetes are progressive. If blurry vision continues, it may result into a more long-term complication as well as a sign of a more serious problem.
Long-term
Consistently high blood sugar could lead to damaged blood vessels, resulting in the most serious diabetes related vision problems called Diabetic Retinopathy.
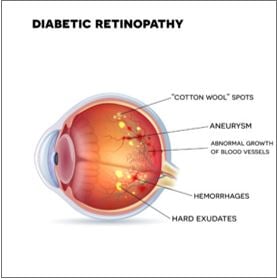
Diabetic retinopathy is a general term used for all disorders of the retina caused by diabetes. The disease progresses through four stages:
- Mild nonproliferative retinopathy
- Moderate nonproliferative retinopathy
- Severe nonproliferative retinopathy
- Proliferative diabetic retinopathy (PDR)
If diabetic retinopathy is not treated and monitored, it can cause serious vision problems and even lead to diabetic macular edema (DME). DME causes a buildup of fluid (edema) at the macula, also known as yellow spots, that appear near the retina. It’s the most common cause of vision loss among people with diabetic retinopathy.
Glaucoma
Other than diabetic retinopathy, glaucoma is another long-term issue that can arise from diabetes. According to the ADA, people with diabetes are twice as likely to suffer from glaucoma than people without diabetes. The longer someone has had diabetes; the more common glaucoma is. Often associated with increased blood pressure, glaucoma occurs when pressure builds up in the eye. Overtime, the retina and the nerve become damaged and cause vision loss.
If left untreated, glaucoma can result in peripheral vision loss and eventually, central vision will also be affected until vision is totally lost. As of now there is no cure for glaucoma, and vision lost from it is irreversible. However, the sooner the glaucoma is caught, the more effective treatment can be to slow down its development. There are also vitamins and supplements that can help prevent or slow down glaucoma, listed in our blog ‘3 Eye Vitamins That May Help Prevent Glaucoma’. If you think you might have Glaucoma, make sure to check with your doctor.
Cataracts
According to the National Eye Institute, adults with diabetes are two to five times more likely to develop cataracts than those without diabetes.
Symptoms of cataracts include:
- Cloudy, blurred, or faded vision.
- Excessive glare or a “halo” around lights.
- Poor night vision.
- Frequent changes in prescriptions.
- Double vision.
Early symptoms of cataracts may be treated with new eyeglasses, brighter lighting, and magnifying glasses. Read more facts about Cataracts in our blog ‘Learn the Facts About Cataracts’.
Steps to Take to Preserve Eyesight
Regular visits to an ophthalmologist can greatly help people with diabetes maintain their vision and keep it in good shape. People who already have a diabetic eye disease may need to make more frequent visits to monitor its development.
Other ways to preserve your eyesight are:
- Keeping blood sugar levels under control.
- Frequently monitoring blood pressure and keeping it at a healthy level.
- A healthy lifestyle, including a clean diet and exercise.
Want to learn more? Read our blog, 'Diabetes and Vision: Can Diabetes Affect Your Eyesight?' or download our free oral health and diabetes guide by clicking the image below.
Want to have Solstice benefits? Call our sales team at 877.760.2247 or email Sales@SolsticeBenefits.com
Already have Solstice benefits? See your plan details by going to https://www.mysmile365.com/ or calling us at 1.877.760.2247.




comments